New Report Details Affordable Care Act Resources and Flexibility for States
New Report Details Affordable Care Act Resources and Flexibility for States
Affordable Care Act Has Made $2.8 Billion Available to States in Implementing Affordable Care Act
The U.S. Department of Health and Human Services (HHS) today released a new report showing that the Affordable Care Act provides states with significant flexibility and resources to improve health care benefits and protect consumers. Already, the law has provided or offered $2.8 billion in funding to states. This is a fraction of the total funding available under the law to help states implement new consumer protections, expand health coverage, and improve health care quality.

HHS Secretary Kathleen Sebelius
“The Affordable Care Act is built on the foundation of providing states with the resources and flexibility they need to build a better, more affordable health care system,” said HHS Secretary Kathleen Sebelius. “This report shows that states have what they need to continue putting comprehensive health insurance reforms in place.”
Prior to the enactment of the Affordable Care Act, the fractured health care system placed tremendous financial burdens on states. In 2008, for example, states spent $17.2 billion on uncompensated care due to the large number of Americans without health insurance. Rising health care costs have also had a significant impact on state budgets.
The Affordable Care Act builds on ongoing state efforts to reform health care, and provides states with new tools, flexibility, and resources to provide their residents with health care benefits and consumer protections at an affordable price. At a time when states are struggling with budget deficits, these resources are providing governors, state legislators and regulators, and the people they serve, with vital assistance to improve lives and reduce costs.
The law also empowers states to choose a variety of implementation strategies to reflect their different insurance markets, provider networks, and the needs of their residents. Under the law, states receive substantial flexibility and financial support to cover the cost of creating new competitive insurance marketplaces and extending coverage to more Americans.
…
The full report:
States and the Affordable Care Act: More Funding, More Flexibility
February 25, 2011
Prior to the enactment of the Affordable Care Act, the fractured health care system placed tremendous financial burdens on States. In 2008, for example, States spent $17.2 billion on uncompensated care due to the large number of Americans without health insurance. And rising health care costs have had a significant impact on State budgets.
The Affordable Care Act builds on ongoing State efforts to reform health care, and provides States with new tools, flexibility, and resources to provide their residents the health care benefits and consumer protections they need and deserve at an affordable price. At a time when States are struggling with budget deficits caused, in large part, by the economic recession, these resources are providing Governors, State legislators and regulators, and the people they serve with vital assistance needed to improve lives and reduce costs.
The law empowers States to implement the Affordable Care Act to reflect their insurance markets, provider networks, and the needs of their residents. The law grants States substantial flexibility and financial support to cover the cost of creating new competitive insurance marketplaces and extending coverage to more Americans.
The Affordable Care Act already has provided or offered $2.8 billion in funding to States, which is only a fraction of the funds available under the law to build insurance Exchanges, expand Medicaid eligibility, and expand and improve prevention efforts, as well as additional grants and funds available to States in 2011 and future years. Moreover, independent experts have estimated that by expanding the number of Americans with insurance and reducing the amount States spend to care for the uninsured, the health reform law will save State and local governments between $70 billion and $80 billion from 2014 to 2019.1
This report includes information on the resources that have been and will be made available to States under the Affordable Care Act and important details about States’ discretion to implement the law in a manner that works best for their residents.
Billions of Dollars in Support for States
The Affordable Care Act includes substantial resources for State governments. Thus far, States have received or can access nearly $2.8 billion from the law and will receive billions more in 2011 and subsequent years. For example, a new round of insurance Exchange grants has just been announced, additional funding from the $15 billion Prevention and Public Health Fund will become available, and higher Federal matching payments for Medicaid long-term care will come on line this year and into the future.
Resources Allocated to State Governments from the Affordable Care Act
As Of February 24, 2011
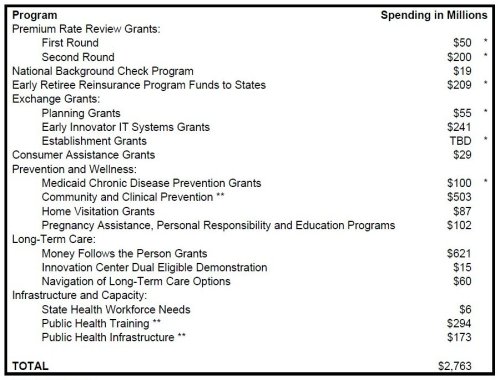

Includes Territories
* Funding announcement has been issued; some of all of the awards have not yet been made.
** Includes funds that would be issues to entities within States; for some programs, funding allocation is
announced but announcements have not yet been issued.
To date, the health law has given States substantial new resources to deliver the benefits of reform to their residents in the form of lower premiums, greater insurance company accountability, and improved health care delivery. This includes:
– Help to Keep Premiums Low: The law provides $250 million to help States and territories improve oversight of proposals by private health insurance companies to raise their rates for small businesses and individuals and families. Since enactment, $45 million has been distributed to 44 States and the District of Columbia and $205 million is now available to States, the District of Columbia and territories to continue those efforts. Early results have shown increased scrutiny of rate increases has helped reduce growth and save consumers and small employers billions of dollars in insurance costs.
– Resources and Tools to Crack Down on Fraud: Nine States have received $19 million in grants to support their development of criminal background checks to safeguard nursing home residents and improve the quality of care. In addition, the Affordable Care Act provides States with new authority to help keep problematic providers from enrolling in Medicaid. The Medicaid Integrity Institute provides free training to State Medicaid agency staff—it conducted 38 courses last year and has trained 1,900 staff since February 2008. HHS is planning a special series of web-based trainings for State Medicaid agencies to share best practices and inform States about new provisions of the law aimed at preventing fraud.
– Reduced Costs for Early Retirees: In 2010, States received a total of $209 million to offset some of their costs of insurance coverage of early retirees and their families. Additional support has already been provided to States this year from the Early Retiree Reinsurance Program (ERRP). This program provides temporary relief for employers and plan sponsors to sustain this coverage until new affordable health insurance choices are available to early retirees and their families in 2014.
– Exchange Grants: More than $296 million worth of grants has been made available to States and territories to start planning for the creation of health insurance Exchanges that will provide affordable private insurance to individuals and small businesses beginning in 2014, and educate residents about their health insurance options. This funding includes “Early Innovator” awards to support six States and a consortium of States in developing an array of models for Exchanges’ information technology systems.
– Support for Consumer Assistance Efforts: Almost $30 million has been awarded to 35 States to support their efforts to establish or strengthen consumer assistance programs that provide consumers with the information they need to pick from a range of health coverage options as well as to provide assistance with enrollment; educate consumers about their rights and obligations; help them appeal decisions when a plan denies coverage; and generally track consumer problems.
– Prevention and Wellness Incentives: States have received grants to improve their community-based wellness programs, to reduce chronic illness, and to tackle problems like smoking. They can now apply for $100 million in grants to create incentives for people in Medicaid to adopt healthy behaviors. And all 50 States have received a portion of the $100 million dedicated to promoting the health of pregnant women and newborns.
– Long-Term Care Support: With additional funding from the Affordable Care Act, all States have now received support for this program to help individuals with disabilities live independently outside of institutions. This month, $621 million in new grants were awarded to 13 States through 2016 for the Money Follows the Person program, joining 29 States that already operate these programs. In addition, one of the first demonstrations launched by the CMS Innovation Center, created by the Act, will promote improved care coordination for people eligible for both Medicaid and Medicare. The law also supports States in providing seniors and individuals with disabilities more options for their health and long-term care services.
– State Capacity: Recognizing that States are on the front-lines in public health response, the Affordable Care Act has already provided over $173 million to improve States’ ability to respond. It also gave grants for State workforce development.
Flexibility to Make Reform Work
The law recognizes that the condition of insurance markets, coverage, and health care systems in general differ in every State. That’s why the Affordable Care Act provides States ample flexibility and options as they implement the key provisions of the Act.
Flexibility / Options Already Taken by States from the Affordable Care Act
As of February 24, 2011

* In other States, there is a Federally-run Pre-existing Condition Insurance Plan
** States applied on behalf of individual market issues in their States given exising State laws.
Under the Affordable Care Act, States have substantial authority to enforce important new consumer protections and benefits. If States choose not to enforce these protections for their residents, HHS will conduct enforcement. To date, every State is currently enforcing the law’s new consumer protections and benefits, since they have the best understanding of their health insurance markets. Some of the new protections and benefits include:
— Banning insurance companies from imposing lifetime limits on the dollar amount they will spend on health benefits, so that people living with chronic conditions and diseases like cancer and diabetes can get the quality care they need;
— Banning insurance companies from dropping coverage just because an individual gets sick;
— Allowing young adults without job-based coverage of their own to stay on their parent’s plan until they turn 26. So far, 2.4 million young adults, including up to
1.8 million of whom are uninsured, and nearly 600,000 of whom purchase coverage in the individual market, are expected to gain coverage;
— Requiring insurers to spend at least 80 percent of premiums in the individual market and 85 percent of premiums in the large group market on health care, rather than executive salaries and administrative costs, to ensure that consumers get value for their premium dollars;
— Banning insurance companies from refusing coverage to children who have a preexisting health condition, helping up to 72,000 uninsured children gain coverage, and in 2014 banning insurance companies from denying coverage to anyone, regardless of their health status;
— Providing individuals in new health plans with a new right to an independent reviewer of insurance company decisions;
— Eliminating lifetime limits on benefits for millions of Americans and phasing out the use of annual limits for all Americans by 2014; and
— Requiring new health plans to cover recommended preventive services – like mammograms, colonoscopies, and immunizations – without charging a deductible, copayment or coinsurance.
– Health Insurance Exchanges: States have tremendous flexibility to dictate the design and operation of the new competitive marketplaces – health insurance Exchanges – that will provide affordable private insurance to individuals and small businesses beginning in 2014. For example, States can:
— Choose to operate an Exchange or to allow the Federal government to create one for their State;
— Choose whether to allow all companies to offer insurance in the Exchange or to select only plans that improve the quality and affordability of the choices; and
— Decide the type of plans that can be offered in the Exchanges, including high-deductible plans and plans associated with Health Savings Accounts (HSAs).
– Pre-existing Condition Insurance Plan: The law provides $5 billion to create the Preexisting Condition Insurance Plan (PCIP) to provide coverage to uninsured Americans who have been excluded from the private insurance market because of a pre-existing condition. States can choose to operate their own PCIP, paid for with Federal funding, or have the Federal government operate a plan for them. Twenty-seven States are operating their own PCIP; 23 States opted for the federally-administered plan.
– Protecting Consumers’ Premiums: States may apply for adjustments to the medical loss ratio (MLR) standard in the individual market, which requires insurers to spend at least 80 percent of premium dollars on health care benefits and activities that improve the quality of care, as opposed to such administrative costs as overhead, salaries and advertising. If a State believes that the new MLR rules will, in the short-run, destabilize its individual insurance market and cause coverage to be less accessible to consumers, it can apply for an adjustment to the MLR requirement to fit the needs of its market. Such adjustments will be available through 2014. To date, four States have applied for this adjustment. In addition, States that required individual market issuers to offer policies with annual limits below those set forth in the new regulations can apply on behalf of those issuers for a temporary waiver of the new minimum annual limits. Four States have been approved for these waivers on behalf of their issuers.
– Taking Advantage of New Medicaid Options: The Affordable Care Act provides new options for States, several of which are accompanied by higher Federal matching payments such as the Health Home option that supports care coordination activity for people with chronic illness and the Community First Choice program that supports community-based health and long-term care for individuals with disabilities. It also allows States to expand coverage to low-income citizens up to 133 percent of the Federal poverty line. So far, two States and the District of Columbia have taken this option. This builds on existing Medicaid flexibility to:
— Modify Benefits: While some benefits, such as hospital and physician services, are required to be provided by State Medicaid programs, many services, such as prescription drugs, dental services, and speech therapy, are optional. States can generally change optional benefits or limit their amount, duration or scope through an amendment to their State plan, provided that each service remains sufficient to reasonably achieve its purpose. In addition, States may add or increase cost sharing for services within limits.
— Manage Care for High-Cost Enrollees More Effectively: Just one percent of all Medicaid beneficiaries account for 25 percent of all expenditures. Initiatives that integrate acute and long-term care, strengthen systems for providing long-term care to people in the community, provide better primary care for children with significant health care needs, and lower the incidence of low-birth weight babies are among the ways that States have improved care and lowered costs.
— Purchase Drugs More Efficiently. In 2009, States spent $7 billion to help Medicaid beneficiaries afford prescription drugs. States have broad flexibility to set their pharmacy pricing.
— Assuring Program Integrity. According to the Department’s 2010 Financial Agency Report, the three-year weighted average national error rate for Medicaid is 9.4 percent, meaning that $33.7 billion in combined Federal and State funds were paid inappropriately. The Federal government and States have a strong, shared interest in assuring integrity in every aspect of the program, and there are new options and tools available to States.
The Price of Repeal
The Affordable Care Act creates a powerful partnership between States and the Federal government that is already strengthening our health care system and helping to ensure millions of Americans have access to quality, affordable health care choices. Still, some want to repeal or “de-fund” the law and return to the days when insurance companies, not patients and doctors, were in control of the health care system. Such action would take away precious resources from States at a time of fiscal challenge and leave their citizens with fewer choices, higher costs, and less protection.
_________
1 John Holahan, Stan Dorn, What is the Impact of the Patient Protections and Affordable Care Act on the States? Urban Institute, June 2010.
…
The report can be found at www.HealthCare.gov/center/reports/states02252011a.pdf
* The above story is reprinted from materials provided by USA Department of Health and Human Services (HHS)
** More information at USA Department of Health and Human Services (HHS)