Therapy Repairs Ravaged Immune System
Therapy Repairs Ravaged Immune System
Gene therapy can safely restore immune function in children with severe combined immunodeficiency and allow some to stop taking painful weekly injections. The finding, from a small clinical trial, offers hope for children born with this deadly condition.
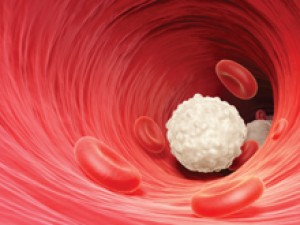
Children with severe combined immunodeficiency (SCID) can’t produce healthy microbe-fighting white blood cells called lymphocytes. As a result, these children are susceptible to a wide range of infections. Most die by the age of 2 if untreated.
One type of SCID arises from a faulty gene for the enzyme adenosine deaminase (ADA). Without this enzyme, toxic compounds build up in the body and inhibit the production of lymphocytes. Once- or twice-weekly injections of ADA can partly restore immune function. But this therapy is expensive and must continue for a lifetime.
For 2 decades, researchers have been exploring an alternative approach that uses gene therapy to replace the damaged ADA gene in the blood-forming stem cells found in bone marrow. But they’ve had trouble developing a method that effectively raises ADA levels and leads to lasting improvements in immune function.
An 11-year effort to test 2 different gene therapy regimens was led by Dr. Donald B. Kohn of the University of California, Los Angeles, and Dr. Fabio Candotti of NIH’s National Human Genome Research Institute (NHGRI). The research was supported in part by several NIH components, including the National Heart, Lung and Blood Institute (NHLBI). The results appeared on September 11, 2012, in the online edition of Blood.
Ten patients with ADA-deficient SCID were treated at either the NIH Clinical Center or the Children’s Hospital Los Angeles. Blood-forming stem cells were isolated from their bone marrow. The cells were treated with retroviral vectors, which delivered healthy ADA genes. The corrected cells were then infused back into the patients’ bloodstream.
The first 4 patients remained on ADA replacement therapy throughout the gene therapy procedure and follow-up. Although the gene therapy had no negative effect, it didn’t improve ADA function. The scientists suspect that ongoing enzyme replacement therapy might have diluted the numbers of corrected lymphocytes in the patients’ immune systems. As a result, the corrected cells couldn’t establish themselves.
For the 6 additional patients, the doctors modified the treatment. Enzyme-replacement therapy was stopped before the procedure, and patients received low-dose chemotherapy, which depletes bone marrow stem cells. “This step proved to be important,” says Candotti. “By adjusting the chemotherapy dosage, we found its optimal level for enhancing the efficacy of the corrected stem cells.”
Three children who received the refined procedure have had improved health for up to 5 years and haven’t needed enzyme replacement injections. The other 3 patients didn’t have lasting improvements from the procedure. Now that the scientists have identified a regimen that can be effective, 8 children have been added to a second phase of the study.
“We are encouraged by the outcome of our gene therapy trial,” Candotti says. “We will continue to follow the progress of our patients and to enroll those who can benefit from this promising gene therapy strategy.”
###
* The above story is reprinted from materials provided by National Institutes of Health (NIH)
** The National Institutes of Health (NIH) , a part of the U.S. Department of Health and Human Services, is the nation’s medical research agency—making important discoveries that improve health and save lives. The National Institutes of Health is made up of 27 different components called Institutes and Centers. Each has its own specific research agenda. All but three of these components receive their funding directly from Congress, and administrate their own budgets.