Toxin Kills HIV-Infected Cells
Toxin Kills HIV-Infected Cells
An HIV-specific poison can kill cells in which the virus is still reproducing despite antiretroviral therapy, a study in mice showed. Such targeted therapies could become a tool in strategies to combat HIV.
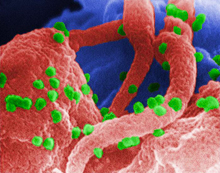
Electron micrograph of HIV (colored green) on human lymphocytes. Image by C. Goldsmith, P. Feorino, E. L. Palmer, and W. R. McManus, courtesy of CDC.
Antiretroviral drugs, used to treat people infected with HIV, don’t eliminate the virus. These drugs suppress HIV, often to undetectable levels, allowing infected people to lead longer and healthier lives. However, because traces of HIV remain in the body, infected individuals can still transmit the virus and must continuously take antiretroviral drugs to maintain their health.
Researchers have been searching for a targeted poison that could complement antiretroviral therapy by killing HIV-infected cells. A genetically designed, HIV-specific poison known as 3B3-PE38 was created in 1998 in the laboratories of Dr. Edward A. Berger of NIH’s National Institute of Allergy and Infectious Diseases (NIAID) and Dr. Ira Pastan of NIH’s National Cancer Institute (NCI). This immunotoxin targets HIV-infected cells and, when taken inside cells, shuts down protein synthesis and triggers cell death.
For the new study, the NIH researchers teamed with Dr. J. Victor Garcia and colleagues at the University of North Carolina School of Medicine, where the experiments were performed. Their work appeared in PLOS Pathogens on January 9, 2014.
The scientists studied 40 mice that were bioengineered to have a human immune system. The mice were infected with HIV. After several months, the mice were given a combination of antiretroviral drugs for 4 weeks. Half the animals subsequently received a 2-week dose of the 3B3-PE38 immunotoxin to complement the antiretrovirals, while the other half continued receiving antiretrovirals alone.
Compared to antiretrovirals alone, the addition of the immunotoxin significantly reduced the number of cells with detectable virus in multiple organs. It also lowered the level of HIV in the blood.
These and previous findings suggest that immunotoxin treatment, when added to antiretroviral therapy, could help keep HIV in remission. The ultimate goal for such treatments would be to eliminate or control HIV infections well enough to allow people to live without a lifetime of continuous antiretroviral therapy.
“This study shows that it’s possible to attack and kill hidden HIV-infected cells that standard therapy can’t touch,” Garcia says. While these results provide a proof of concept, much study will need to be done before the approach could be used in the clinic.
By Harrison Wein, Ph.D.
![]()
###
* The above story is reprinted from materials provided by National Institutes of Health (NIH)
** The National Institutes of Health (NIH) , a part of the U.S. Department of Health and Human Services, is the nation’s medical research agency—making important discoveries that improve health and save lives. The National Institutes of Health is made up of 27 different components called Institutes and Centers. Each has its own specific research agenda. All but three of these components receive their funding directly from Congress, and administrate their own budgets.