A Better Test for Kidney Function
A Better Test for Kidney Function
Kidney function can be estimated more precisely by measuring blood levels of both creatinine and cystatin C than by using either marker alone, a new study found. The technique could help doctors more accurately diagnose chronic kidney disease.
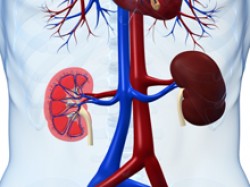
The kidneys filter your blood, removing waste and extra water to make urine. The kidney’s filtration rate, called the glomerular filtration rate (GFR), reflects how well the kidneys are filtering. Accurate estimates of the GFR are important for identifying kidney disease, which often has no symptoms until just before the kidneys fail. An estimated 23 million American adults may have chronic kidney disease. They could take steps to protect their kidney function if their kidney disease were detected early.
The standard way to estimate GFR has been to measure blood levels of creatinine. Creatinine is a waste product from the digestion of dietary protein and the normal breakdown of muscle tissue. However, creatinine levels can be affected by several other factors, including diet, muscle mass, malnutrition and other chronic illnesses. One potential alternative is to measure cystatin C, which is produced by cells throughout the body and removed from blood by the kidneys.
A research team led by Dr. Lesley Inker at Tufts Medical Center in Boston aimed to develop better models for estimating GFR by taking into account both creatinine and cystatin C. To test their models, the researchers gathered data on a diverse group of over 5,000 people from 13 studies that measured kidney function. The work was funded by NIH’s National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
The team reported in the New England Journal of Medicine on July 5, 2012, that GFR estimates based on a creatinine-cystatin C equation provided the most precise and accurate results. The improvement was greatest when estimates of GFR were near 60—the usual threshold for diagnosing chronic kidney disease. Among people whose estimated kidney function was between 45 and 74 based on creatinine, the combined equation correctly reclassified to 60 or greater 17% percent of those who had been estimated to have a GFR under 60. The combined equation also appeared less subject to differences in age, sex or diabetes status.
“The new creatinine-cystatin equation is more accurate over a broader range of kidney function and body size, and less altered by other medical conditions,” Inker says.
Further study will be needed to understand how best to use these tests in the clinic. The addition of cystatin C testing would likely increase laboratory costs. Screening based on creatinine alone might prove sufficient for initial testing.
###
* The above story is reprinted from materials provided by National Institutes of Health (NIH)
** The National Institutes of Health (NIH) , a part of the U.S. Department of Health and Human Services, is the nation’s medical research agency—making important discoveries that improve health and save lives. The National Institutes of Health is made up of 27 different components called Institutes and Centers. Each has its own specific research agenda. All but three of these components receive their funding directly from Congress, and administrate their own budgets.