Organ Transplants and Cancer Risk
Organ Transplants and Cancer Risk
November 21, 2011
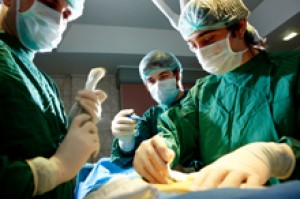
Organ transplant recipients have a high risk of developing 32 different types of cancer, according to a new study. Future research to understand why may lead to better strategies for preventing cancer among transplant recipients.
In 2010, over 28,000 organ transplantations were performed in the U.S., including 16,899 kidney, 6,291 liver, 2,333 heart and 1,770 lung transplants. Transplant recipients are known to be at a higher risk for developing cancer than the general population. But past studies of cancer risk in transplant recipients focused mainly on those who received kidney transplants. Other studies were too small to accurately estimate risk for all but the most common cancer types.
For a more comprehensive look, a research team led by Dr. Eric A. Engels of NIH’s National Cancer Institute (NCI) evaluated medical data from more than 175,000 transplant recipients—about 40% of all organ transplant recipients in the country. Their report appeared in the November 2, 2011, issue of the Journal of the American Medical Association.
The researchers found a twofold overall increased risk of cancer among transplant recipients. They noted elevated risk for 32 different types of cancer, some known to be related to infectious agents (such as anal cancer and Kaposi sarcoma) and others unrelated to infections (such as melanoma and thyroid cancer). The most common cancers among transplant recipients were non-Hodgkin lymphoma (14% of all cancers in transplant recipients), lung cancer (13%), liver cancer (9%) and kidney cancer (7%).
The risk of cancer was affected by the type of transplant. Lung cancer risk, for example, was highest in lung recipients. Smoking-related disease is often the reason for a lung transplant, and lung cancer typically arises in the remaining diseased lung rather than the transplanted one. The risk of liver cancer was elevated only among liver recipients. That might be partly explained by hepatitis B or C infection in the transplanted liver or by the fact that diabetes is common among transplant recipients. The risk of kidney cancer, in contrast, increased for all recipients.
“While transplantation is a life-saving therapy for patients with end-stage organ disease, it also puts recipients at an increased risk for developing cancer, in part because of medications administered to suppress the immune system and prevent rejection of the organ,” Engels says. “The cancer risk among transplant recipients resembles that of people with HIV infection, whose risk is elevated for infection-related cancers due to immunosuppression.”
The researchers now plan to focus on the cancers that occur at higher rates among transplant recipients. They aim to discover how medical conditions and immunosuppressive medications contribute to cancer risk. “In addition, we hope our findings will stimulate other research into the carcinogenic mechanisms associated with organ transplantation,” Engels says.
###
* The above story is reprinted from materials provided by National Institutes of Health (NIH)
** The National Institutes of Health (NIH) , a part of the U.S. Department of Health and Human Services, is the nation’s medical research agency—making important discoveries that improve health and save lives. The National Institutes of Health is made up of 27 different components called Institutes and Centers. Each has its own specific research agenda. All but three of these components receive their funding directly from Congress, and administrate their own budgets.