Medical Miracle: When Serendipity Meets Science
Medical Miracle: When Serendipity Meets Science
This week we’re breaking from our regular format to share a serendipitous patient care story.
The video (and text) below relay an incredible account of a how a chance meeting between a cardiologist and neurosurgeon helped to give a brave, young mother a new lease on life.
…
…
Serendipity that struck not once, but twice, may have saved 32-year-old Jamie Arliss’ life.
Two years ago Arliss, a licensed practical nurse, was working at a medical practice near her hometown of Clyde, N.Y. At the time, the staff was learning to perform electrocardiograms (EKGs) and practicing on each other. When it was her turn, the test results were “a little odd and everyone said it was probably nothing,” she recalled.
Arliss had suffered progressive fatigue, limiting her ability to exercise or complete tasks that required significant physical activity.
“I always felt tired and short of breath, and I’d get chest pains sometimes. My doctor would order blood tests and they’d come back normal every time,” said Arliss, who is raising a 15-year-old daughter. “I quit smoking, started taking vitamins more regularly and paying attention to myself, but it continued.”
After the unusual EKG, however, Arliss couldn’t ignore the results and was persistent in learning what was behind them. As it turned out, University of Rochester Medical Center cardiologists found a rare tumor in her heart.
“This was an extraordinary tumor, so unusual, so rare that we couldn’t find any information about how to treat it anywhere in our extensive research,” said Christopher Cove, M.D., assistant director of the URMC Cardiac Catheterization Laboratory. The only information available came from autopsy reports, which showed similar growths but offered no clues for treating them.
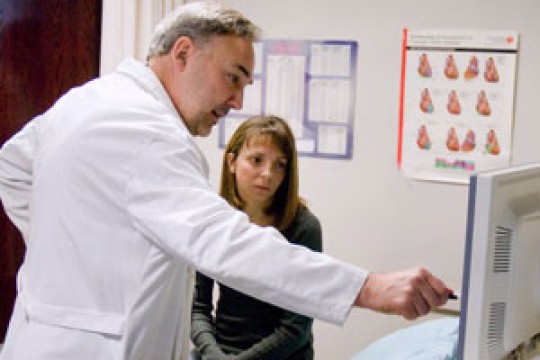
Arliss consulting with Christopher Cove, M.D., about treatment of the rare tumor that was found in her heart.
A medical mystery
Cardiothoracic surgeon H. Todd Massey, M.D., studied images of the mass after it was discovered in fall 2008.
“It was nothing I’d ever seen before,” said Massey, senior transplant surgeon for the URMC Program in Heart Failure and Transplantation. Initially, he was concerned that it was cancerous. Luckily, a biopsy proved otherwise.
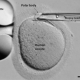
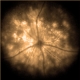
Massey later identified it as an arterio-venous malformation (AVM), a circulatory malfunction that can form anywhere in the body, often in the brain and lungs. When an AVM extends outside an artery or organ, creating a mass, it’s called a tumor. In Arliss’ case, it grew into a benign tumor the size of a golf ball along the lateral wall of her heart.
Typically, doctors would try to remove the mass, or to cut off its blood supply through coil embolization or radiation therapy. But Massey couldn’t remove it surgically because it would damage too much of Arliss’ heart muscle. He suggested interventional cardiologists use a common coil embolization procedure, which would clogs the vessels, block blood flow, and starve the tumor.
That was unsuccessful because the tumor was complex and deeply rooted in the heart.
“If you cut off one blood supply, it was able to find another one to let the tumor continue to grow,” Cove said.
And the life-threatening tumor kept growing indeed, eventually reaching 3.5 centimeters and beginning to spread outside of the left ventricle. Considering that the average heart is the size of a fist, the tumor was immense.
Doctors recommended Arliss consider joining the list for a heart transplant – a daunting prospect for the woman who wanted to continue her nursing education and raise a teen daughter with her husband, Scott.
An unlikely team
Finding nothing in the medical literature about AVMs in the heart, URMC cardiologists continued reaching out to colleagues across the country for advice and consideration. They shared the initial images of the mass, which were later published in the Journal of theAmerican College of Cardiology in April 2010. While there was curiosity about the discovery, none of their peers offered suggestions.
About the same time, URMC neurosurgeon Babak Jahromi, M.D., Ph.D., was in the midst of a renovation project and temporarily moved his clinical suite into the cardiac catheterization center. Cove and other interventional cardiologists had the chance to observe one of Jahromi’s techniques for treating brain disorders – including AVMs.
Jahromi regularly treats cerebral AVMs by “liquid embolization” – a procedure using a tiny catheter to inject Onyx, a glue-like substance, into the tumor to shut down the vascular growth, destroy vessels and stop the tumor in its tracks. Intrigued, Cove and Jahromi began studying the possibility of using the same substance to destroy the mass in Arliss’ heart.
“Cardiologists and neurosurgeons both use minimally-invasive catheterization techniques to treat diseases, so it was a great opportunity for cross-fertilization between our specialties.”
Jahromi knew there would be a learning curve.
“This was a completely different ball game for me,” admitted Jahromi, assistant professor of Neurosurgery, Imaging Sciences and Neurology. He typically uses the liquid embolization procedure to treat masses that are measured in millimeters – not centimeters or inches. The massive heart tumor required the use of 10 times the amount of Onyx that he would normally use in the brain.
“It was a beating heart that continued to move as you inserted the catheter and delivered the therapy. And we did it all while the patient was awake,” Jahromi said. “But that’s what the cardiologists do, so both of us working together we were a good combination.”
Experts believe the Dec. 9 procedure was the first time the glue-like substance and technique were used in the heart.
Repeated imaging tests showed the Onyx filling the space, with no additional activity at the tumor site. The now-inert mass could remain there for the rest of her life, but will no longer draw blood from Arliss’ heart nor impair her heart function, Cove said.
Arliss is regaining strength and endurance and has returned to work in the medical office. Doctors continue to monitor her recovery and heart function, and will study what happens to the now-dead mass in her heart.
“We’re very pleased that Jamie will have no long-term effects from this procedure,” Cove said. “She’ll move on and enjoy a good quality of life from here.”
###
* The above story is adapted from materials provided by University of Rochester Medical Center
![]() ______________________________________________________________________
______________________________________________________________________