Regeneration of specialized cells offers hope for treating chronic kidney disease, researchers say
Regeneration of specialized cells offers hope for treating chronic kidney disease, researchers say
Damage to podocytes — a specialized type of epithelial cell in the kidney — occurs in more than 90 percent of all chronic kidney disease. Now researchers at the Stanford University School of Medicine have uncovered an unexpected pathway that reveals for the first time how these cells may regenerate and renew themselves during normal kidney function.

This finding is an important step toward one day therapeutically coaxing the cells to divide, which could be used to treat people with chronic kidney disease.
“Researchers have studied these cells for years, but the prevailing view has been that they don’t renew themselves,” said associate professor of medicine Steven Artandi, MD, PhD. “Now we’ve found that podocytes can enter and leave the cell cycle in response to certain common signaling pathways.”
Artandi is the senior author of the study, published online Dec. 4 in Nature Medicine. The first author of the work is former postdoctoral scholar Marina Shkreli, PhD, who is now at the Laboratory of Biology and Pathology of Genomes at the University of Nice in France.
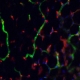
Podocytes are found only in the kidney and are an integral structural component of its blood-filtering system. They stand shoulder-to-shoulder in a part of the organ called the glomerulus and wrap their long “feet” around the semi-permeable capillaries through which blood flows. Narrow slits between the feet allow small molecules, such as water and salts, to pass while blocking large proteins.
This filtering process is the first step to forming urine, and it is critically important — even one missing cell can leave a gap that would allow unwanted molecules through the barrier. (Imagine wrapping your hands around a length of leaky garden hose so that the water seeps out between your fingers. Lift up one finger and you’re liable to get sprayed in the face.)
This may be why previous researchers searching for signs of self-renewal in podocytes were unsuccessful, because any such renewal or replacement would likely need to be carefully orchestrated to avoid compromising the filtration system. As a result, scientists have been forced to conclude that the podocytes rarely, if ever, divided.
“It used to be thought that you were born with podocytes, and you died with the same podocytes — you don’t make any more during your lifetime,” said Artandi. The only exception was certain rare types of kidney disease in which the podocytes abandon their blood-filtration duties en masse to de-differentiate into less-specialized, dividing cells that little resemble their predecessors. As a result, the glomerulus collapses and the patients’ kidneys begin to fail. One such disease is HIV-associated nephropathy, or HIVAN.
The problem was, such a scenario doesn’t make a lot of evolutionary sense — particularly when other epithelial cells routinely regenerate themselves. “Podocytes are vitally important, and are also under enormous physical stress,” said Artandi. “It’s hard to understand why we would have such a vulnerable blood-filtration system.”
To understand more about kidney biology, Artandi and Shkreli investigated the role of a protein component of the telomerase complex called TERT. Although telomerase is best known as an enzyme involved in cell aging, recent research in Artandi’s lab and others have shown that TERT also plays a role in many types of cellular regeneration.
The researchers found that temporarily increasing the expression of TERT in adult, otherwise healthy laboratory mice caused the formerly stolid podocytes to abruptly de-differentiate and begin dividing. As a result, the glomerulus collapsed in a way that resembles what happens in humans with HIVAN. Conversely, ceasing the overexpression allowed the cells to stop dividing, re-specialize and resume their normal functions.
When Artandi and Shkreli looked closely at the glomeruli in humans with HIVAN, they found that TERT expression was increased. Equally important, the Wnt signaling pathway, which is important in embryonic development and in the self-renewal of stem cells, was also activated. (Previous research in the Artandi lab has linked telomerase activity to the Wnt pathway.) Blocking Wnt signaling in a mouse model of HIVAN also stopped the podocytes from dividing and improved their function.
“The implication is that podocytes may utilize recognized pathways of regeneration to renew themselves throughout life,” said Artandi. People suffering from chronic kidney disease may simply have worn out or outpaced their podocytes’ capacity for renewal, he believes.
Now that the researchers know podocytes have the ability regenerate in response to common cellular signals, their next step is to learn whether this regeneration occurs in healthy animals and people. “If we can harness this regeneration,” Artandi said, “we may one day be able to treat people with chronic kidney disease.”
In addition to Artandi and Shkreli, other Stanford researchers involved in the study include medical resident Kavita Sarin, MD, PhD; graduate students Matthew Pech and Peggie Cheung; medical student Woody Chang; lab manager Stephanie Brockman; former research assistant Eunice Lee; research associate Frank Kuhnert, PhD; and associate professor of medicine Calvin Kuo, MD, PhD.
The research was funded by the National Institutes of Health, the Stanford School of Medicine, the Stanford Center on Longevity and the Glenn Laboratories for the Biology of Aging at Stanford.
###
Steven Artandi. Bio.

Steven Artandi
Associate Professor, Medicine – Hematology
Hematology Clinic
300 Pasteur Dr
A175 MC 5312
Stanford, CA 94305
Member, Bio-X
Member, Cancer Center
Associate Professor (By courtesy), Biochemistry
> Clinical Focus
Cancer> Hematology
Medical Oncology
> Honors and Awards
Fellow, American Association for the Advancement of Science (AAAS) (2008)
> Professional Education
Medical Education: Columbia University NY USA (1995)
Residency: Massachusetts General Hospital MA (1997)
Fellowship: Dana-Farber Cancer Institute MA (2000)
Ph.D., Columbia University Microbiology (1995)
M.D., Columbia University (1995)
A.B., Princeton University Chemistry (1986)
> Current Research Interests
Telomeres, the nucleotide repeats that cap the ends of eukaryotic chromosomes, serve critical roles in promoting cell viability and in maintaining chromosomal stability. In humans, telomeres shorten progressively with cell division and aging because DNA polymerase cannot fully replicate the extreme ends of chromosomes. Critical telomere shortening and loss of the protective telomere capping function in cell culture initiates senescence and crisis responses that profoundly alter chromosome stability, cell cycle progression and survival. Expression of telomerase, the reverse transcriptase that synthesizes telomere repeats, is sufficient to lengthen and stabilize telomeres, thus enabling cells to proliferate in an unlimited fashion. Telomerase is expressed in stem cells and progenitor cells in self-renewing tissues, is downregulated with differentiation and upregulated in the vast majority of human cancers. In the Artandi lab, we are interested in unraveling the molecular and cellular mechanisms according to which telomeres and telomerase modulate stem cell function and carcinogenesis.
TERT and STEM CELLS
Telomerase is comprised of two subunits: TERT, the telomerase reverse transcriptase, and TERC, the telomerase RNA component. In stem cell and progenitor cell compartments, TERT serves a critical role in maintaining telomere length and function to support tissue homeostasis. However, TERT serves an additional function in stem cells, distinct from its role in telomere lengthening. Using a conditional transgenic mouse system, we recently showed that TERT can promote proliferation of quiescent epidermal stem cells. Induction of TERT in mouse skin caused a rapid transition in hair follicle from the resting phase (telogen) to the active phase (anagen) of the hair follicle cycle and robust hair growth. We showed that this novel function for TERT was independent of TERC and therefore independent of TERT’s previously understood role in telomere synthesis. We are actively investigating this non-canonical function for TERT in stem cell populations.
TISSUE REGENERATION AND AGING
Aging in humans and other mammals is associated with impaired proliferative responses in settings of stress, suggesting that altered stem cell function may underlie certain aspects of aging. We are interested in understanding how stem cells self-renew and differentiate and how TERT modulates stem cell function. We showed that conditional activation of TERT causes stem cells to proliferate, leading to a new anagen cycle. By promoting the developmental switch to anagen, TERT led to robust hair synthesis. We are actively investigating the effects of TERT on other adult stem cell compartments and pursuing the mechanism of TERT action through diverse appraoches.
CANCER AND CHROMOSOME INSTABILITY
Telomeres shorten profoundly during the early stages of human carcinogenesis due to insufficient levels of telomerase. Marked telomere shortening is evident even in the pre-invasive pathological stages of epithelial cancer development in humans. We showed previously that telomere dysfunction impairs cell survival via activation of the tumor suppressor p53. In mice that lack both telomerase and p53, this checkpoint function is abrogated, allowing increased cell survival in the setting of worsening telomere function. Telomere dysfunction in the absence of the p53 checkpoint promotes spontaneous cancer in epithelial organs, including breast cancer, skin cancer and colon. We are interested in generating mouse models of human cancer in which telomere shortening promotes cycles of chromosomal instability to understand the earliest stages of cancer development. We have a specific interest in breast cancer, which is the most common malignancy in women. Our laboratory is investigating the role of mammary stem cells in breast cancer through the creation of novel mouse models that will reproduce the chromosomal instability seen in human breast cancer.
###
* Stanford University Medical Center integrates research, medical education and patient care at its three institutions – Stanford University School of Medicine, Stanford Hospital & Clinics and Lucile Packard Children’s Hospital.
** The above story is adapted from materials provided by Stanford University School of Medicine
________________________________________________________________